
21 May The Role of Psychology in Chronic Pain Management: How Mental Health Support Transforms Recovery
Chronic pain affects millions of Australians every year and can touch nearly every part of daily life. It’s not just a physical problem—long-lasting pain often brings stress, sleepless nights, and emotional exhaustion. That’s why more people are turning to approaches that address both the body and the mind.
Modern pain care now goes further than medication or physical treatment alone. Support from psychologists, pain specialists, and allied health professionals can make a real difference. Cognitive behavioural therapy, mindfulness, and group support are just a few of the proven methods that help people cope with pain.
What is Chronic Pain?
Chronic pain is more than just an ache that lingers after an injury or illness; it’s a persistent discomfort that continues for months or even years. This type of pain doesn’t serve as a useful warning signal for the body as acute pain does—instead, it often remains long after tissues have healed.
Defining Chronic Pain
Chronic pain is typically any pain that lasts longer than three months, beyond the usual course of recovery. It can show up anywhere in the body—back, neck, joints, or as headaches. Unlike short-term pain, which usually has an identifiable cause and end point, chronic pain sometimes appears without a clear reason. Living with persistent pain is exhausting and confusing because it doesn’t always make sense to the person experiencing it.
Impact on Daily Life and Work
Dealing with chronic pain affects more than just the area that hurts. It can:
- Make simple everyday tasks, like walking or getting dressed, much harder.
- Lower productivity at work or force a change in jobs.
- Disrupt hobbies, social events, and family activities.
- Lead to financial stress due to missed work or medical expenses.
Chronic pain can quickly turn routine days into tough challenges. People often find themselves weighing every activity against the pain, which can feel isolating.
The Connection Between Chronic Pain and Mental Health
Pain does not just attack the body—it takes a toll on the mind, too. Long-term pain is linked to feelings of frustration, sadness, anxiety, and hopelessness. Constant discomfort can disturb sleep and drain emotional resources. Over time, this can snowball into depression or chronic stress, making it even harder to manage pain.
Psychological support is key. Addressing the mental side of pain is just as important as physical treatment, if not more so. That’s why approaches that bring together medical, psychological, and physical therapies can help break the cycle of pain and distress.
The Need for a Multidisciplinary Approach
Managing chronic pain is rarely a one-person job. The most effective care teams include doctors, physiotherapists, psychologists, and sometimes pain specialists, all working together. This multidisciplinary approach doesn’t just tackle the pain itself; it also helps with the ways pain disrupts sleep, mood, and relationships.
A team-based strategy gives people access to treatments like exercise therapy, medications, counselling, and education about pain science. If you want more insight into effective local care options, explore available Chronic pain treatment Brighton for guidance.
The Psychological Factors Affecting Chronic Pain
The Mind-Body Connection in Pain Perception
Pain isn’t only a signal from the body—it passes through the filter of your mind. Your thoughts, beliefs about pain, and life experiences all shape how pain feels. For example, if you expect something to hurt or remember past pain, your brain can actually amplify those sensations.
Studies show that negative thought patterns (like catastrophizing, where you expect the worst outcome) make pain seem stronger and longer-lasting. On the other hand, people who approach pain with a positive or solution-focused mindset often report less intense symptoms. The way we think sets the stage for how our bodies react.
Our memories matter, too. If you’ve had a traumatic or deeply uncomfortable experience with pain in the past, your brain can hold onto that, making new pain feel even worse. This doesn’t mean the pain isn’t real—it’s very real—but your mind helps interpret every signal coming from your body.
The Role of Emotions and Mental Health
Emotions are tightly linked to physical pain. Feeling upset, anxious, or hopeless doesn’t just make you feel “blue”—it can ramp up the volume on pain signals. This is because chronic stress pours stress hormones like cortisol into your system, keeping your nerves on high alert.
Many people with chronic pain will say their worst days are often their most stressful or lonely. Pain and mental health influence each other and can easily feed into a cycle:
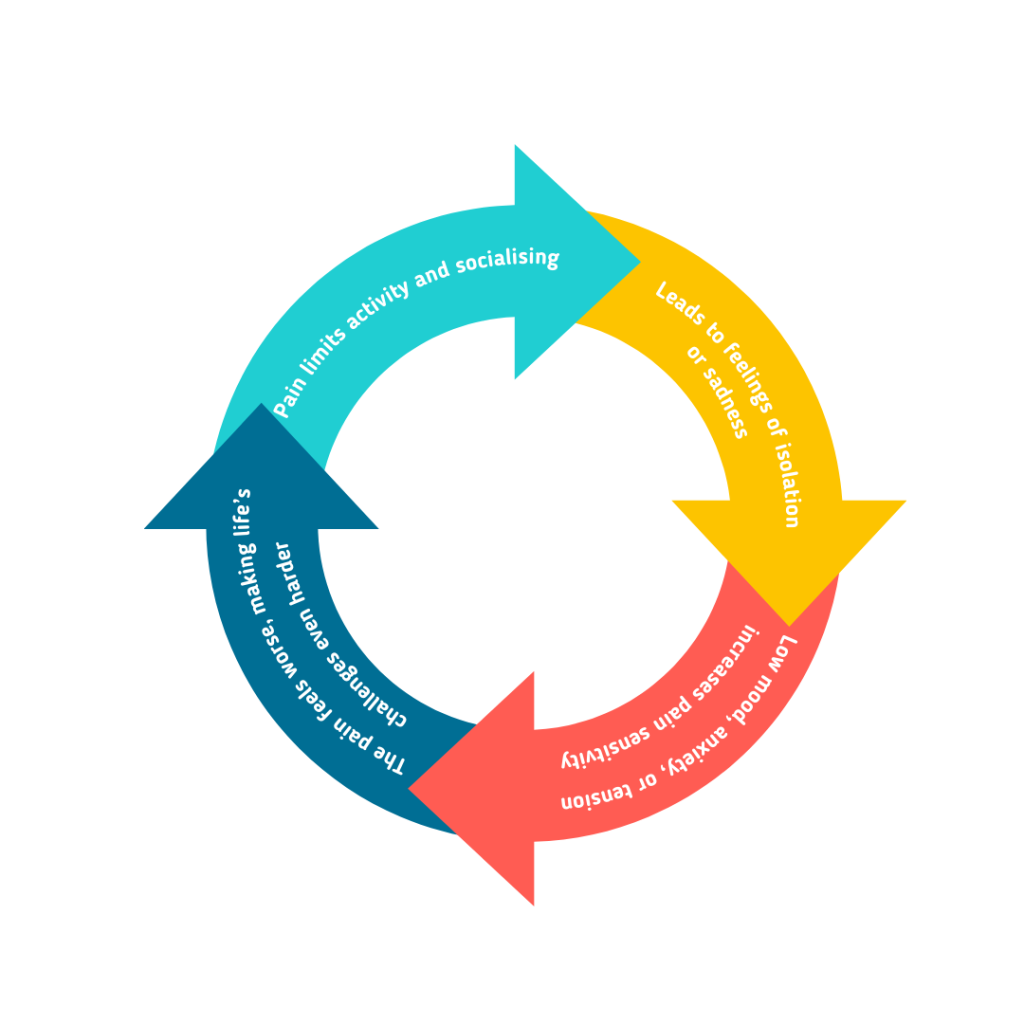
- Ways mental health impacts pain:
- Stress raises pain perception and worsens sleep.
- Anxiety can create muscle tension, leading to more pain.
- Depression can sap motivation, making movement and self-care difficult.
The link between poor sleep and pain is also important. When you’re tossing and turning at night, your body misses time to repair and reset. Simple changes—like working with an allied health team to improve sleep—can make a difference. Explore Improving sleep with allied health for tips on better rest and pain management.
By tackling both the emotional and physical sides of pain, you take real steps toward living better—even with chronic discomfort.
Evidence-Based Psychological Interventions for Chronic Pain
When living with chronic pain, mental habits and emotions play a huge part in your overall well-being. Psychological therapies have been proven to reduce pain intensity, improve mood, and help people handle the challenges of daily life. These approaches teach practical ways to manage difficult thoughts and feelings tied to pain, building confidence and restoring a sense of control.
Cognitive Behavioural Therapy (CBT) for Pain
CBT is one of the most well-researched therapies for chronic pain. Its main idea is simple: your thoughts, feelings, and actions are all connected. If you can change how you think about pain, you can change how you feel and how you react to it.
People with chronic pain often get stuck in unhelpful thinking patterns:
- Catastrophizing (“This pain will never end”)
- Hopelessness (“Nothing I do helps”)
- Fear of movement (“If I move, I’ll make it worse”)
CBT helps break this cycle. How?
- Challenging unhelpful thoughts: You learn to spot negative thinking and replace it with more balanced, realistic ones.
- Building coping skills: Techniques like pacing activities, goal setting, and problem-solving support daily routines.
- Reducing avoidance: Facing feared activities in gradual steps can actually boost confidence and reduce distress.
Mindfulness and Relaxation Techniques
Mindfulness and relaxation strategies are practical tools that help you relate to pain differently. Mindfulness teaches you to pay attention to the present moment—without trying to change anything or judge your experience. Over time, these skills help you respond to pain with less stress and more calm.
Common approaches include:
- Mindfulness meditation: Sitting quietly and noticing thoughts, sensations, or feelings as they come and go.
- Deep breathing: Slow, controlled breaths calm the nervous system, lower muscle tension, and reduce pain intensity.
- Progressive muscle relaxation: Tensing then relaxing each muscle group helps lower body tension and can ease pain signals.
- Guided imagery: Using visualisation to picture a peaceful scene, which distracts from pain and reduces anxiety.
These techniques are simple yet powerful. Practiced regularly, they can cut down emotional distress, improve sleep, and even help the body handle physical discomfort more effectively.
The Role of Psychologists in Pain Management Teams
Psychologists are a vital part of the pain management team. They bring expert knowledge about how thoughts, behaviours, and emotions influence pain. Their job is not just “counselling”—they teach evidence-based tools that allow people to take an active role in managing their pain.
In a multidisciplinary setting, psychologists work side-by-side with doctors, physiotherapists, and other health professionals. They support patients to:
- Understand their pain from a biological and psychological view
- Learn coping strategies that fit their personal situation
- Set goals for daily function and recovery
- Address mood or anxiety issues tied to chronic pain
The value of a team approach is that it looks at the whole person, not just the symptom. Integration with other allied health professionals leads to better results for many patients.
None of these techniques claim to “cure” pain, but it gives you tools to manage pain and improve quality of life.
When to Seek Psychological Support for Chronic Pain
Recognising when to ask for help with chronic pain can be just as important as managing the pain itself. Many people try to tough it out, hoping things will get better on their own. This can lead to more frustration, distress, and even a worsening of symptoms. Psychological support isn’t just for when you’re at your breaking point—it can make a meaningful difference even early on, sometimes turning things around before they spiral.
Common Signs You Might Need Psychological Support
It’s normal to have good and bad days with chronic pain, but certain signs suggest you might benefit from talking to a psychologist or counsellor. These signs aren’t about weakness—they’re signals your mind and body need an extra hand.
Look out for any of these signs in yourself or someone you care about:
- You feel constantly sad, hopeless, or anxious because of your pain.
- Sleep doesn’t come easily, or you wake up still feeling tired and restless.
- Pain is making it hard to work, look after loved ones, or take care of yourself.
- You’ve lost interest in hobbies or activities you once enjoyed.
- Frustration or anger comes up often, and it’s hard to control your mood.
- Friends or family mention that you seem withdrawn, irritable, or have changed.
- You’ve started relying on alcohol, drugs, or other substances to cope.
- You worry your pain means something very serious, even though tests show nothing new.
If one or more of these sounds familiar, it may be time to consider psychological support. Spotting these patterns early helps prevent the emotional impact of pain from snowballing.
Why Early Help Makes a Difference
Reaching out for psychological assessment or therapy as soon as problems start can be a game-changer for recovery. When you act early, you’re more likely to:
- Learn healthy coping strategies before habits like isolation or avoidance take hold.
- Address sleep or mood problems that make pain worse.
- Reduce the risk of depression, anxiety, or substance use taking over your life.
- Keep work, relationships, and self-care on track.
It’s always easier (and more effective) to build healthy habits early, rather than rescue things when they’ve already fallen apart. Think of psychological support as another tool in your kit—like exercise, medication, or seeing a physiotherapist. They all work best together.
Meet the Psychologists at Brighton Spine and Sports Clinic
Living with chronic pain means carrying more than a physical burden. It’s a daily challenge that can test your resilience, strain your relationships, and impact your mood. At Brighton Spine and Sports Clinic, the approach to pain management is rooted in understanding the whole person. That’s why our team includes skilled psychologists who specialise in helping people regain control and confidence, even when pain tries to take centre stage.
Who Are the Psychologists?
Brighton Spine and Sports Clinic is home to two experienced psychologists, Leah Levy and Robert Postlethwaite, with a deep understanding of chronic pain and mental health. Their backgrounds blend evidence-based psychology with practical strategies to support recovery. They focus on chronic pain, anxiety, depression, stress, and the mental side of living with ongoing physical symptoms.
You can get to know more about their professional journeys, training, and values by visiting the Meet Our Specialists page. There, you’ll find their credentials and how their unique experience shapes the care they provide every day.
Conclusion
Psychological support gives people living with chronic pain more than just comfort—it provides proven tools to handle tough days and break the hold that pain can have on mind and body. Taking care of your mental health alongside physical treatment builds true, long-term strength. Working with caring professionals, learning new skills, and forming healthy habits helps you move forward, even when things get challenging.
Treating both body and mind creates a path toward a better life with fewer limits. Taking a holistic approach, like building strong routines and adopting positive brain health habits found in Brain health tips and lifestyle modifications, can bring extra relief and hope.
If you’re ready to reclaim more of your life from pain, start by embracing both physical and psychological support. Small steps today can make tomorrow brighter. Thanks for reading—your effort to learn and take action is a strong move toward real change.
It is important to note that the specific interventions and strategies employed by any medical practitioner will depend on the individual’s unique needs. Each practitioner in a care team will work collaboratively with each other to provide comprehensive care and support for the individual.
If there is a part of your condition or injury that you are struggling to understand, be sure to seek clarification with your medical professional. None of the information in this article is a replacement for proper medical advice. Always seek advice from your trusted medical professional regarding your health and/or medical conditions.
