
12 May The Stress-Back Connection: Why Your Nervous System Carries the Work Week
It’s Friday arvo. The laptop is shut, yet your neck still feels tight, your shoulders sit up near your ears, and your low back nags when you stand. That kind of tension isn’t always about posture or injury.
Stress changes the way your nervous system reads safety and threat. When work pressure stays high, the body can start guarding around the spine, even after the work day ends. The Australian Institute of Health and Welfare continues to highlight mental health as a major health burden in Australia, so it makes sense to look at how that load lands in the body too. For many people, psychology, movement, and myotherapy and massage services can work well together.
How stress changes the way your nervous system holds your body
Your nervous system is always scanning for danger. That’s useful when something is truly wrong. However, long work stress can make that system more protective than it needs to be.
When that happens, the body often braces. Muscles around the neck, ribs, shoulders, jaw, hips, and low back tighten to create a sense of control. At first, this can help you push through. After a while, though, the body can get stuck in that guarded setting.

Your brain does not separate deadlines from physical threat
Deadlines, poor sleep, long sitting, conflict, and constant alerts can all push the body into fight, flight, or freeze. In plain terms, the body starts acting like it needs to stay ready.
So breathing gets shallow. The jaw clenches. Shoulders rise. The trunk muscles stay switched on, which can leave the back stiff and sore. Some people also move less freely, and that adds another layer of tension.
That’s why a busy week can lead to real back pain without a clear injury. The pain is real. The trigger just may be stress, not damage.
Why spinal guarding can linger into the weekend
The tricky part is that the stressor can end while the body keeps bracing. A hard meeting finishes, but your system may still act as if it’s happening.
As a result, Saturday can start with tight hips, braced shoulders, and a back that feels cranky when you bend, walk, or sit in the car. You may also feel more sensitive to small aches because the nervous system hasn’t fully settled.
In other words, your body can carry the work week longer than your calendar does.
The signs your work stress may be showing up in your back
Stress-related guarding often follows familiar patterns. These signs don’t diagnose anything, but they can help you notice when pressure is showing up through your spine and muscles.
Common body patterns, from neck tension to low back ache
A few patterns are especially common during hard work weeks:
- Neck stiffness after emails or meetings, often with the head pushed forward.
- Upper back tightness during long sitting, especially when breathing feels shallow.
- Headaches with shoulder tension, or a jaw that feels clenched by the end of the day.
- Low back soreness by Friday, even if you haven’t done heavy lifting.
- Feeling worse when tired or overwhelmed, then easing a bit after rest or a calmer day.
Pain like this is not “all in your head”. It’s still pain. Stress just changes how the system holds, protects, and reacts.
When stress, mood, and pain start feeding each other
This loop can build quietly. Stress increases tension and pain. Then pain affects sleep and mood. After that, poor sleep and low mood make the nervous system more reactive, so the body guards even more.
That link matters because mental strain and physical pain often travel together. If stress, worry, burnout, or low mood are part of the picture, the role of psychologists in pain teams can help explain why mental health support may also ease the physical side.
What helps calm the system and ease back tension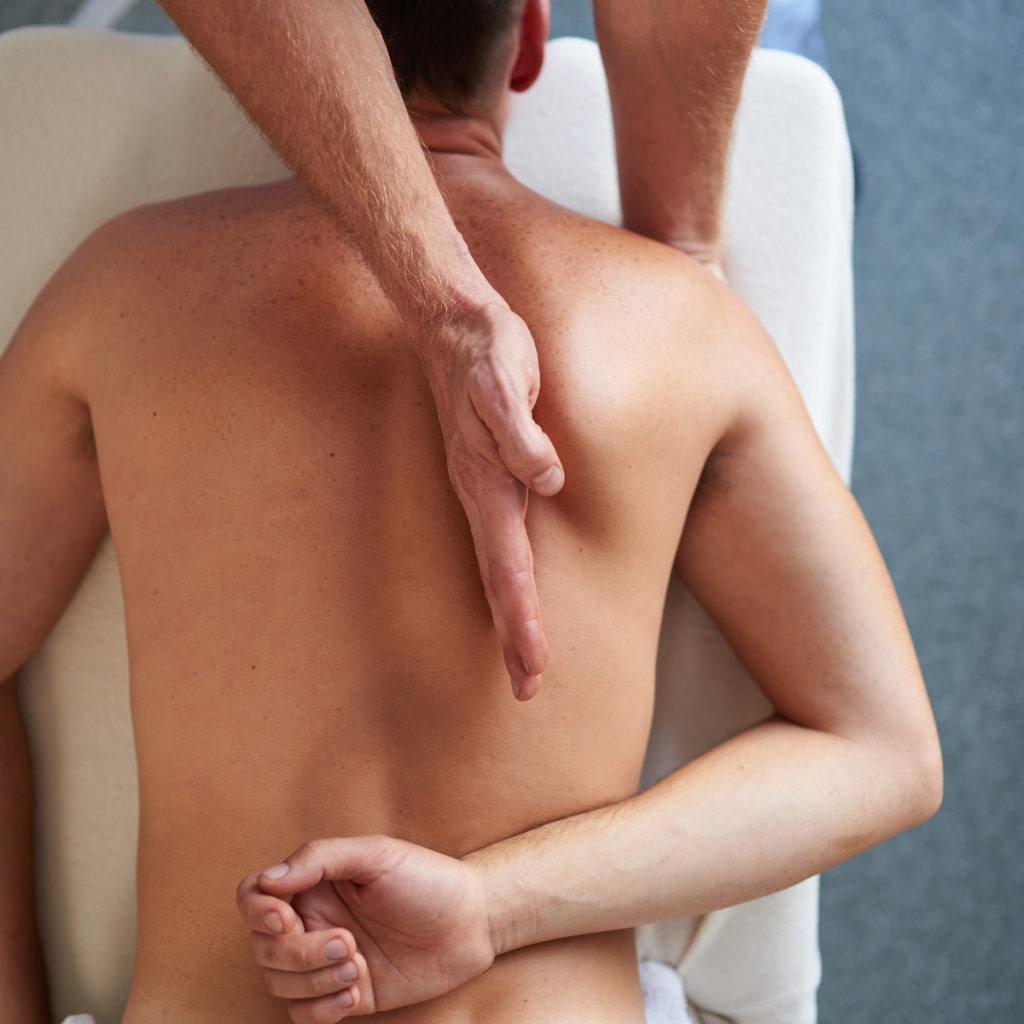
Most people don’t get far by chasing one quick fix. If stress is driving the guarding pattern, it usually helps to work on both the body and the load behind it.
That means easing muscle tension, improving movement, changing work habits, and giving the nervous system repeated signs of safety. Small shifts matter because they happen often.
How myotherapy and remedial massage can help break the guarding pattern
Hands-on care may help reduce muscle tension, improve movement, and give the body a chance to stop bracing for a while. That pause can be useful, because when the system feels safer, movement often feels easier too.
Myotherapy and remedial massage can both support this process. They’re not magic fixes, and they shouldn’t promise cures. Still, matched to the person’s stress load, work habits, and recovery patterns, they can be a helpful part of care. If you want a clearer breakdown, the difference between remedial massage and myotherapy is worth reading.
Small daily habits that tell your body it can let go
You don’t need a perfect routine. You need repeatable signals that tell your body the threat has eased.
Short walking breaks help. So does changing position often instead of chasing one “perfect” posture. Slower breathing can reduce chest and neck tension. Gentle mobility can loosen stiff hips and ribs. Limiting after-hours work helps the brain stop scanning. A steadier sleep routine gives the system time to reset.
If stress has become constant, psychological support can also help, especially when worry, burnout, or low mood are mixed in. Body care tends to work better when the mind gets support too.
Conclusion
Back tension is not always just a posture problem. Sometimes it’s a nervous system that has been holding onto the work week for too long. When you spot that pattern early, you can respond in a smarter way, with physical care, better recovery habits, and support for stress when needed. The goal isn’t to force your body to relax. It’s to help it feel safe enough to let go.
It is important to note that the specific interventions and strategies employed by any medical practitioner will depend on the individual’s unique needs. Each practitioner in a care team will work collaboratively with each other to provide comprehensive care and support for the individual.
If there is a part of your condition or injury that you are struggling to understand, be sure to seek clarification with your medical professional. None of the information in this article is a replacement for proper medical advice. Always seek advice from your trusted medical professional regarding your health and/or medical conditions.
